Newborn screening test developed for rare, deadly neurological disorder
Goal is to speed diagnosis and treatment of Niemann-Pick type C
 U.S. Air Force
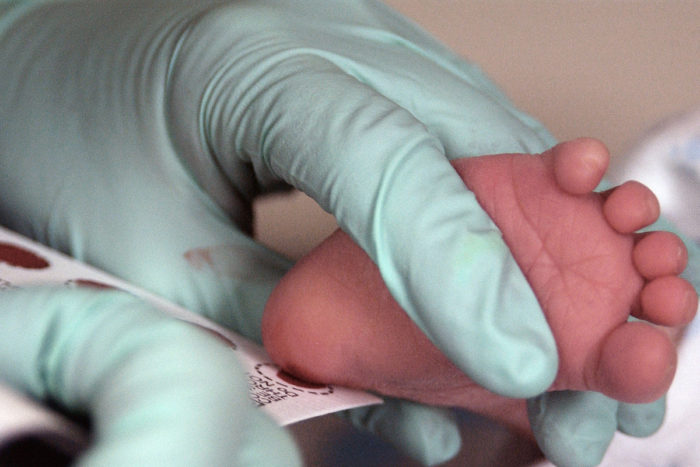
U.S. Air ForceDried blood spots are used to screen newborns for a number of rare inherited conditions. Scientists have developed a new dried blood spot screening test for Niemann-Pick type C, a rare neurodegenerative condition that usually is not diagnosed until after damage to brain cells has begun.
Soon after birth, a baby’s blood is sampled and tested for a number of rare inherited conditions, such as cystic fibrosis and sickle cell anemia. But no such test has existed for a progressive neurodegenerative disease, called Niemann-Pick type C (NPC), that typically is not diagnosed until at least age 2, after neurological symptoms have begun to develop.
Now, a study led by Washington University School of Medicine in St. Louis describes a newborn screening test that identifies infants with NPC, an often fatal condition in which cholesterol builds up and eventually destroys brain cells. While there is no cure, early detection and treatment with disease-modifying therapies eventually may save lives and improve prospects for managing the disease in the future.
The research appears May 4 in the journal Science Translational Medicine.
According to the study, the screening test meets all federal requirements for clinical laboratory testing. The investigators verified the accuracy of the screen by testing it on more than 5,000 dried blood spot specimens. Of these, 44 were known to be samples from NPC patients; 134 were samples from people who were known carriers; and the remaining 4,992 were control samples from people without the condition. Using a two-tiered testing strategy, the new test quickly identified all of the NPC patients with no false positives and no false negatives.
The progressive loss of brain cells in NPC causes severe developmental disabilities. Life expectancy varies, with affected individuals typically succumbing to the disease by the second decade of life. Treatment with miglustat, an inhibitor of lipid synthesis that is approved outside the U.S. for treatment of NPC, has shown evidence of slowing disease progression.
Senior author Daniel S. Ory, MD, and his colleagues currently are evaluating in clinical trials a compound called cyclodextrin that has proved an effective treatment in animal models of NPC. When administered directly into the space surrounding the spinal column, cyclodextrin causes a release of the cholesterol trapped inside the brain cells of NPC mice and cats, reducing neuronal damage and prolonging survival in the animals up to eightfold.
“We wanted to develop a newborn screen for NPC because we know that the earlier we intervene with investigational treatments in animal models of the disease, the longer the animals live,” said Ory, the Alan A. and Edith L. Wolff Professor of Cardiology. “If we can identify infants with NPC early, we could direct these children to clinical trials, potentially beginning treatment before they have begun to show symptoms of neurological damage, hopefully slowing disease progression and improving quality of life.”
With collaborators at the New York State Department of Health, Ory and colleagues have begun to transition the newborn screening test from the laboratory to the state screening facility. The plan is over the next few years to perform a trial run to assess the ability of the test to prospectively identify newborns with NPC. The pilot program will include specimens from babies whose parents have given permission for the blood samples to be used for research. The investigators said the infants participating in the pilot program won’t undergo any additional blood sampling since the new screening test is designed to utilize the standard dried blood spot samples already collected from all babies born in the United States.
With miglustat therapy available off-label in the U.S. and potential therapies in clinical trials, the researchers said their goal is to see the test added to the recommended uniform screening panel defined by the U.S. Department of Health and Human Services (HHS). Newborn screening programs vary by state, but most include the disorders recommended by the HHS, and many states test for additional diseases.
“One of the considerations for adding a new test to the recommended screening panel is whether we can do anything for patients once they are identified,” Ory said. “Many of these drugs, including cyclodextrin, are still in the experimental stages. But in the context of clinical trials, we do have therapies to offer NPC patients.”
The new test measures levels of a bile acid produced by the liver. The researchers suspected bile acids might make good markers for early detection of NPC because these compounds are waste products of cholesterol processing, which is abnormal in these patients. The researchers showed that NPC patients have about thirtyfold higher amounts of this bile acid in the blood than healthy individuals. Importantly, levels of this bile acid also could distinguish between patients with NPC and carriers of the disease who show no symptoms.
In the two-tiered testing strategy, the first-tier screening run returns results in about two minutes, according to the researchers. Ory said the first run must be short to make screening feasible for hundreds of samples per day. If any results are ambiguous in the quick test, the second tier test gives results in about seven minutes. Ory said of the more than 5,000 samples they tested, only one required the longer test to clarify an uncertain result.
Despite the complexity of the science behind the test, Ory speculated it would be no more expensive to run this new test than other standard newborn screening tests.
“These types of tests can be quite automated,” he said. “If you’re running 500 samples per day, you can test many specimens at once at robotic handling stations that many state lab facilities already have. The cost of materials and labor would be on par with current accepted newborn screening tests. Once established, a reasonable estimate of the cost of running these tests would be less than $1 per sample.”
While cases of NPC are rare, Ory pointed out that the benefits of studying rare diseases can extend beyond patients with the condition.
“In studying what causes NPC and how it progresses, we learn more about normal cholesterol metabolism,” Ory said. “Cyclodextrin is being developed as a drug for NPC, but it currently is being tested in the laboratory in other much more common conditions, including atherosclerosis and Alzheimer’s disease. The drug has shown positive results in recent studies of mouse models of these diseases. Those researchers would not be studying cyclodextrin if not for the initial work that was done by the NPC community.”